Guiding the future of cardiometabolic care l Gerald Watts
Guiding the future of cardiometabolic care

Winthrop Professor Gerald F Watts is globally recognised for his pioneering research in cardiometabolic medicine.
Cardiovascular disease is a leading cause of premature death in Australia, with diabetes, lipid disorders and chronic kidney disease being major risk factors.
There are an estimated 100,000 people with familial hypercholesterolaemia (FH) in Australia. Before advances in cardiometabolic medicine, inherited lipid disorders such as FH (which includes high LDL or ‘bad’ cholesterol) were under diagnosed, poorly understood, and had limited therapeutic options. This resulted in delayed treatment, preventable health complications and inequities in care.
At the heart of a growing health challenge
Professor Gerald Watts is a Winthrop Professor of Cardiometabolic and Internal Medicine at The University of Western Australia (UWA) and Senior Consultant Physician at Royal Perth Hospital. He is globally recognised for his pioneering research in cardiometabolic medicine, including diabetes, obesity, kidney disease, inherited lipid disorders, and arterial disease treatment, with a focus on the prevention and treatment of cardiovascular disease, including FH. In recognition for his sustained contributions to cardiovascular medicine, lipid disorders and diabetes, he was awarded in 2003 a Doctor of Science by Imperial College, University of London.
His interest in the field was shaped by personal experience. His family has a history of diabetes, FH, and premature coronary heart disease, his brother having his first heart attack at 48 years of age and mother having her first cardiovascular event at the age of 54. He developed a strong commitment to understanding the metabolic and genetic drivers of cardiovascular disease.
Over more than four decades, Professor Watts has dedicated his career to improving outcomes for patients at high cardiometabolic risk, translating research into clinical practice, education, health system innovation and policy at both national and international levels.
“FH is a tier 1 and the most actionable monogenetic condition in the world. Untreated, the risk of coronary heart disease is very high but is greatly diminished through early treatment.”
Professor Gerald Watts, UWA
New ways to detect and treat disease early
As early as the 1980’s, Professor Watts’ research demonstrated how high urinary albumin levels could be used to detect the risk of diabetic renal disease and hypertension. This work led to the development of a clinical biomarker and screening tool, now routinely used to identify individuals at risk of kidney disease in diabetes, and cardiometabolic kidney disease.
In 1992, Professor Watts published one of his most influential work, St Thomas’ Atherosclerosis Regression Study (STARS) trial. This landmark contribution employed one of the first computerised, highly precise methods for assessing angiographic evidence of changes in coronary arteries. The trial showed that lowering lipids through dietary intervention or diet plus medication could halt or reverse abnormalities in the arterial walls, called atherosclerotic plaques, of the coronary arteries in participants with hypercholesterolemia. It also presaged the development of modern LDL lowering therapies, including statins and PCSK9 inhibitors, informing future national and global LDL focused guidelines.
The research was also seminal in informing a number of earlier coronary disease prevention guidelines, culminating in more recent ones including:
- The American Heart Association Diet and Lifestyle Recommendations
- National Cholesterol Education Program
- 2019 and 2025 European Society of Cardiology ESC/EAS Dyslipidaemia Guidelines
- 2023 UK NICE Cardiovascular disease: risk assessment and reduction, including lipid modification (NG238)
- 2023 WHO Saturated & Trans fat Intake Guideline
- 2023 International Atherosclerosis Society guidance for implementing best practice in the care of familial hypercholesterolaemia
By 1997 his research had expanded to investigate the mechanisms linking lipid disorders, diabetes, obesity, and cardiovascular disease. He and his team, principal collaborators being Dr Dick Chan and Professor Hugh Barrett, developed stable isotope, tracer techniques to study how lipoproteins are produced, transported, and cleared in the body. Their technique was highly innovative and unique, with few groups worldwide undertaking comparable work at the time. Their work showed how therapies such as statins, fibrates, fish oils and weight loss regulate lipid-related risk factors for cardiovascular disease. For clinicians, this insight meant a clearer rationale for treatment options and supported shared decision making with patients. Their research was supported by multiple grants from the National Health and Medical Research Council (NHMRC) and the National Heart Foundation of Australia.
Later, the team provided the scientific rationale for including treatments such as PCSK9 inhibitors, used to lower LDL (“bad”) cholesterol and when standard therapies are insufficient it underpinned scientifically the adoption of PCSK9 inhibitors in Australia, which formed the basis for national clinical guidelines and models of care for Familial Hypercholesterolaemia.
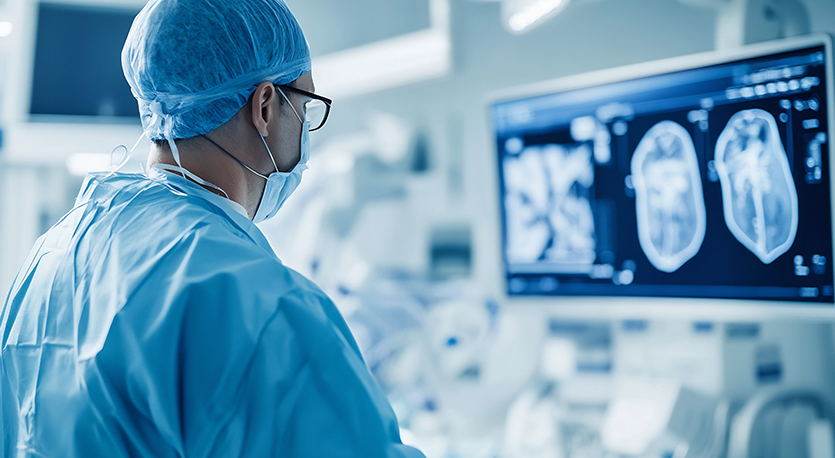
Angiographic evidence from the research informed a number of coronary disease prevention guidelines.
Building innovative models of care
In 2000, prompted by visiting UK cardiovascular genetics expert Professor Steve Humphries, Professor Watts redirected his research toward interventions for individuals at the highest risk of cardiometabolic disease, particularly FH.
Alongside his research programme, Professor Watts is an active clinician and served as Head of Internal Medicine at Royal Perth Hospital, where he led clinics in cardiometabolic disorders, lipid disorders, hypertension, and general medicine.
Cascade testing
From 2008, Professor Watts co-led with leaders from the Department of Health of Western Australia, a three year pilot study with the Western Australian Department of Health involving experts in laboratory medicine at PathWest, geneticists, clinicians, nursing staff, health psychologists, health economists, and patient advocates. It demonstrated cascade testing of relatives was an accurate and cost effective approach for early detection of FH. The first documented, co-ordinated cascade testing program for FH in Australia, it identified large numbers of previously undiagnosed cases, who achieved substantial LDL cholesterol reductions with statins plus other medications and lifestyle changes, and were projected to reduce heart attacks. This work and review supported the Royal Australasian College of Pathologists’ proposal for the introduction of genetic cascade testing as a Medicare Benefits Schedule item in 2020.
“The clinical service was highly cost effective and saved lives, and it improved patient quality of life for people who were treated early.”
Professor Gerald Watts, UWA
Familial Hypercholesterolaemia Western Australia (FHWA) Model of Care
Historically, FH had been relatively underdiagnosed and inadequately treated, with no national strategy. Introduced in 2010 and implemented by the Department of Health of WA in 2011, the FHWA Model of Care provided a comprehensive framework to manage cases, by integrating specialist lipid clinics, genetic testing, cascade screening, and risk notification. Developed by Professor Watts and his collaborators with the FH Australasia Network (within the Australian Atherosclerosis Society), in 2011 it became the foundational framework for FH care across Australia and New Zealand, influenced international guidance in Europe and the United States, and informed the International FH Foundation models of care. The approach was expanded into general practice and paediatric services recognized in 2014 by a WA Health Executive Award. The state and national guidelines informed in 2023 a major guidance from the International Atherosclerosis Society on the integration and implementation of care for FH.
National Familial Hypercholesterolaemia Registry (FH Australasia Network)
Established in 2006 by the Australian Atherosclerosis Society, the FH Australasia Network co-ordinates the collection of data on FH care across Australia, with Professor Watts serving as its Chair. In 2017, he led the design of the FH Australasia Network Registry (FH Registry) which supports GPs, nurses, and specialist teams in the identification, diagnosis and treatment of FH, with corresponding implementation, service and patient outcomes. Support for the FH Registry was provided by the NHMRC and the pharmaceutical industry. The database is hosted by the UWA University Library and is managed by Dr Jing Pang, the curator of the registry, from the UWA Medical School.
“I am passionate about how implementation science can change clinical practice, ensuring that new therapeutic advances efficiently translate into real-world clinical settings across Australia and globally.”
Professor Gerald Watts, UWA
New models of care guide medical professionals in the detection and treatment of FH
Gene silencing
Professor Watts has played a major role in testing and evaluating novel RNA-based treatments for complex, inherited lipid disorders, including:
- Elevated Lipoprotein(a), Lp(a), a type of ‘bad’ cholesterol, which is six times more toxic to the artery than FH, but cannot be lowered with current medication or lifestyle measures. Reduction in Lp(a) requires administering an injection that inhibits the mRNA of Lp(a) in the liver. Three significant clinical trials have been completed, and two cardiovascular outcome trials are currently underway.
- Familial Chylomicronemia Syndrome (FCS) / Multifactorial Chylomicronemia Syndrome (MCS), in which the the body is unable to clear triglycerides (fat) that accumulate in and damage the pancreas, can lead to life-threatening haemorrhagic pancreatitis. These conditions are difficult to manage, require highly restrictive diets, markedly impair quality of life, and are poorly responsive to standard drug therapies.
Professor Watts and his team worked with biotechnology partners including Arrowhead Pharmaceuticals and Amgen in the United States, and Novartis based in Switzerland. They showed that by silencing the disease causing APOC3 messenger RNA with an injection every three months triglyceride levels were reduced by about 80%, resulting in a lower incidence of acute pancreatitis. This demonstrated the potential of gene silencing approaches to address previously untreatable metabolic diseases. Patients are now receiving therapy through an early access program at Royal Perth Hospital. The team is now progressing toward testing one-time gene-editing treatments to permanently lower in the blood the proteins that cause very high triglycerides and its consequences, portending a major advance in precision medicine.
“We are already delivering gene silencing therapies for high impact disorders like FCS and MCS, that you can only treat in a few expert centres worldwide.”
Professor Gerald Watts, UWA
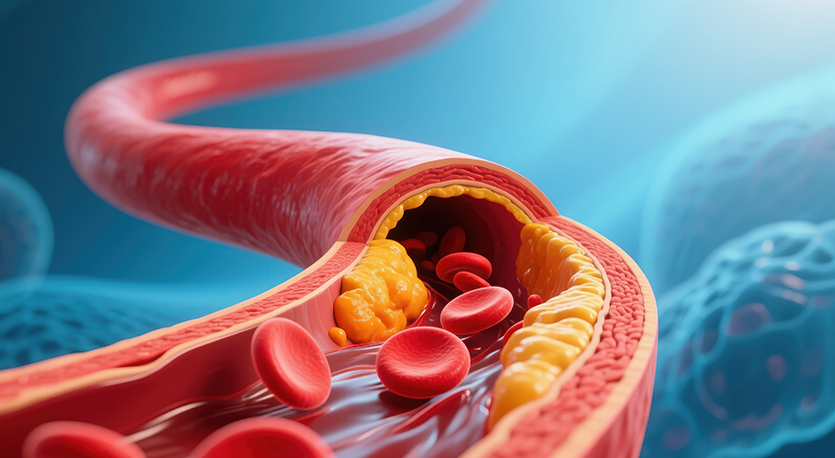
Complex inherited lipid disorders need specialised treatment
Implementation and Extension of Care of FH
Implementation of care was extended beyond specialist and public sectors through collaborations with primary care professionals, including GPs and nurse practitioners. This required integration of protocols and referral pathways, supporting equitable metropolitan and regional care of at-risk patients. Three nurses have transitioned into hospital and community based care. Supported by key collaborators in general practice and NHMRC partnership grants, the team also developed a consensus guidance for GPs.
The team worked with the UWA Rural Clinical School of WA in Bunbury and Albany, and later Geraldton, to establish services and encourage a new approach to preventative cardiology, with funding from the Val Lishman Health Research Foundation. In about 2020, FH-focused clinical services were set up at Fiona Stanley Hospital and at Sir Charles Gairdner Hospital, with support from the FH Australasia Network and RPH Clinic.
From 2018, an NHMRC supported partnership grant with general practice led to a screening intervention that improved detection of individuals at risk of premature CAD , and those suitable for genetic testing. A GP-led 2021 study across 15 clinics showed that as part of routine practice, there were significant LDL cholesterol reductions and improved attainment of treatment goals, alongside evidence that FH screening and management in general practice is cost-effective with substantial health gains.
“I am privileged not only to be involved in teaching and training healthcare professionals and healthcare providers, but also in delivering services in an integrated way, in collaboration with GPs and other specialists and members of the Department of Health of WA, that collectively aims to close the gaps in care.”
Professor Gerald Watts, UWA

Screening and treatment by primary care professionals is vital in managing cardiovascular disease.
Addressing care gaps through co-design
Patients and advocates were central to the research, identifying care gaps, providing lived experience and advocating for access to new therapies. This patient-centred approach led to the establishment of FH Australia, now an independent, patient led advocacy organisation. National studies on the implementation of care were supported by NHF, NHMRC and MRFF grants.
In 2020, an analysis of the FH Registry undertaken in collaboration with an NHMRC-funded research fellow identified a number of gaps in paediatric cardiovascular care. The data showed late diagnosis, high coronary artery disease risk, poor attainment of LDL-cholesterol goals, under-use of cascade testing, and inequities linked to social determinants of health resulting in non-adherence to therapy, such health illiteracy and lower socio-economic status.
Paediatric cardiovascular care
One in five Australians living with FH are children, with more than 90% remaining undiagnosed until adulthood. In recent years, Professor Watts has prioritised early detection and treatment of FH and Lp(a) in children and young adults to improve long‐term outcomes. In 2022, he and his collaborator Dr Andrew Martin (UWA Medical School, Paediatrics) developed a clinical care guide for affected children and adolescents across Australia. The FH Registry includes paediatric patients, helping ensure equitable access to precision, evidence-informed care and well-supported transitions between services. The development of paediatric services has recently been boosted by support from the Perron Foundation. The team is now advocating for a virtual patient hub to better support this cohort and their families.
“FH is a lifetime condition that untreated has a very high burden of coronary artery disease, so the earlier you detect and treat it, the better are the long-term outcomes.”
Professor Gerald Watts, UWA

The earlier FH is detected and treated, the better the outcome.
Recognition and the next generation of discovery
Professor Watts has supervised and trained numerous clinicians and researchers, expanding the cardiometabolic workforce through his roles at UWA and in hospital settings. He consistently ranks as a Highly Cited Researcher placing him among the most influential cardiovascular researchers nationally and internationally. His research contributions have been acknowledged through major honours and invited lectures including: election as a Fellow of the European Society of Cardiology; WA Cardiovascular Alliance 2025 Lifetime Research Achievement Award; MRF; RPH Lifetime Achievement and Mentorship Awards; the Cardiac Society of Australia and New Zealand 2022 RT Hall Prize; and invitation to deliver prestigious named lectures such as the Akira Yamamoto Lecture in the Asia Pacific region and the Myant Lecture in the UK. His work across discovery, translation and implementation has reshaped cardiovascular prevention and positioned Australia at the forefront of precision cardiometabolic care.

